
Unlocking early detection, better treatment pathways for PCOS and endometriosis using microRNAs

The main regulator in PCOS and endometriosis are microRNAs (miRNAs), which are small molecules that act like a bridge between the two conditions, but on a molecular level. Image used for representational purposes only
| Photo Credit: Getty Images/iStockphoto
Two disorders caused by the dysfunction of the reproductive and endocrine system are PCOS (polycystic ovary syndrome) and endometriosis. Both are deeply linked by genetics and how our body regulates certain biological signals.
Polycystic Ovary Syndrome (PCOS) is a hormonal disorder, that affects the reproductive system in women. It leads to irregular menstruation, higher levels of the male hormone androgen, and also causes the formation of chain-like cysts in the ovaries. Delayed diagnosis of PCOS leads to clinical issues including insulin resistance, dyslipidaemia and obesity (body fat level fluctuations), and increases the risk of acquiring cardiovascular issues. In endometriosis, the endometrial tissues grow outside the uterus in other locations of the body, leading to a series of medical issues.
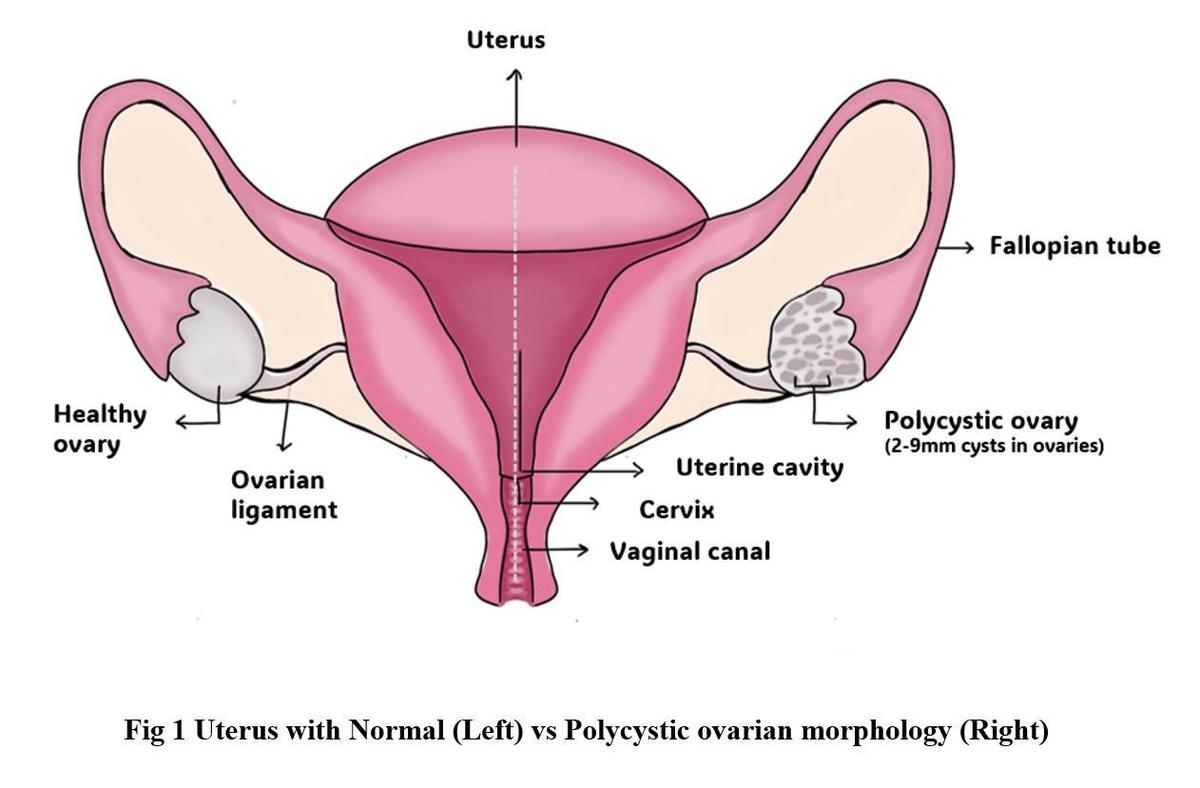
Courtesy, SRIHER
What regulates these conditions?
The main regulator in these conditions are microRNAs (miRNAs), which are small molecules that act like a bridge between PCOS and endometriosis, but on a molecular level. miRNAs are versatile biological controllers that change their behaviour based on the disease. For example, miR-146a, a commonly known microRNA can interfere and change insulin levels, affecting blood sugar and also cause weight issues in PCOS, but in endometriosis, the same microRNA promotes abnormal tissues to grow and form new blood vessels. Another group of miRNAs, the miR-200 family can disrupt the ovarian function in PCOS, while they form painful lesions in endometriosis.
By studying the expression patterns of these miRNAs in biological fluids like blood where they are found in large quantities, doctors can potentially diagnose these conditions well in advance and accurately differentiate them. This is especially important in India, where PCOS cases are significantly higher than the global average affecting 22% of females due to factors such as sedentary urban lifestyles, increased Vitamin D deficiencies and genetics.
Keeping in mind that cases of PCOS are rising rapidly, research focusing on these genetic markers can help medical professionals move from generalised treatments and towards precision medicine, using a simple minimally-invasive blood test to identify risks such as infertility or metabolic disease early and create a personalised care plan that fits a woman’s molecular profile.
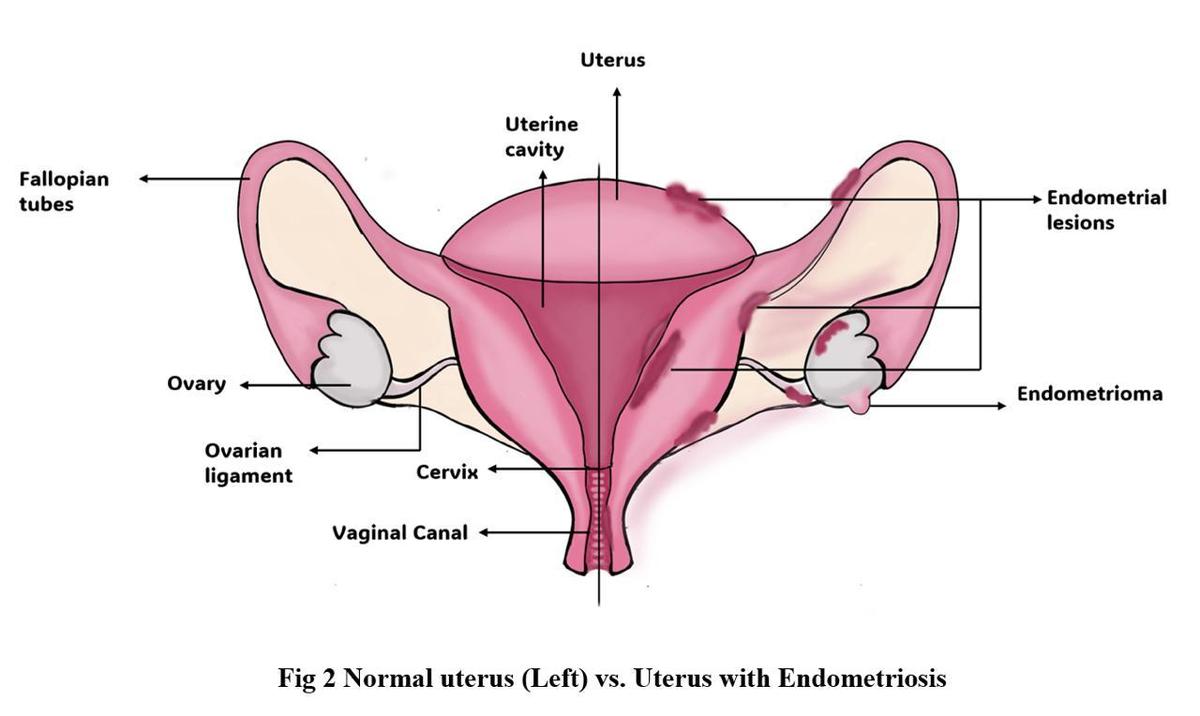
Courtesy, SRIHER
Do the conditions overlap?
Recent research has indicated overlapping miRNA signatures in PCOS and endometriosis, hinting at the overlapping mechanisms of both the conditions. Focusing on the genetic variations specific to the Indian population can help researchers and clinicians understand how miRNA expression differs across different ethnic and geographical groups, effectively helping to improve diagnosis and treatment outcomes. As miRNAs can easily be found in circulating fluids including blood, saliva and urine samples, they offer a way to make precision tests less invasive than options like surgery.

What this means for women
From a research point of view, findings associated with miRNAs in women’s health disorders are a gamechanger because they can allow clinicians to create a molecular profile for every individual. Instead of a one-size-fits-all approach to diagnose and treat PCOS and endometriosis, doctors can use the curated miRNA panels to differentiate between PCOS and endometriosis, diagnose them at a very preliminary stage, and even utilise newer treatment modalities such as antagomirs to ‘switch off’ any harmful mediators, potentially recovering genetic balance.
Most importantly, focusing on PCOS and endometriosis cases in the Indian population can help fill a wide gap in global medical data. Screening and diagnosing these conditions early can effectively reduce the long-term risks associated with the two conditions and help women get the right reproductive treatment and care for better health in the long run.
(Dr. V. Deepa Parvathi is associate professor, department of biomedical sciences Sri Ramachandra Institute of Higher Education and Research. deepaparvathi@sriramachandra.edu.in; Dr. Usha Rani G., is with the department of obstetrics and gynaecology, Sri Ramachandra Institute of Higher Education and Research. usharani@sriramachandra.edu.in)
Published – April 06, 2026 02:16 pm IST








